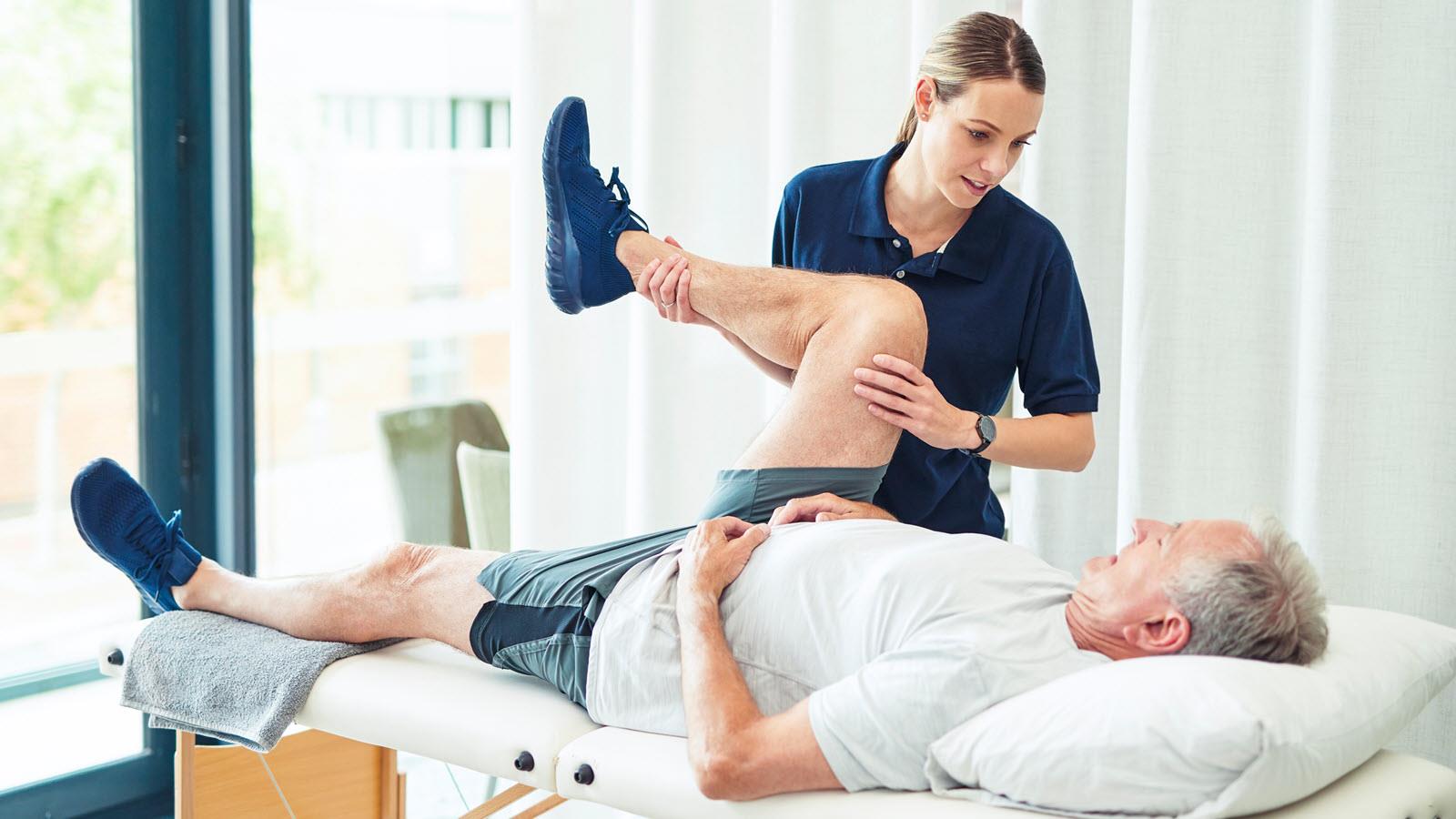
For those who live with bleeding disorders, joint problems can reduce their mobility and keep them from being active. When blood doesn’t clot as it should, bleeds can occur inside joints, causing pain. Older patients are especially affected because they didn’t benefit from treatment advances until later in life. Then they experience the compounding effects of age-related joint problems, like arthritis.
That makes physical therapy an important aspect of health care delivered at Hemophilia Treatment Centers, which are comprehensive clinics that take a holistic approach to the patient’s overall health and well-being. A survey from the National Bleeding Disorders Foundation (NBDF) looked at how closely physical therapists at HTCs are following treatment guidelines from the foundation’s Medical and Scientific Advisory Council (MASC). The council issues annual recommendations for treatments that are evidence based, meaning that research has shown their usefulness and effectiveness.
The current guidelines for physical therapists include frameworks for managing joint health and rehabilitating patients after major bleeds. The guidelines also advise on how best to use cold packs to reduce swelling and when shoe inserts and braces can be most helpful.
But it can take up to 17 years for these guidelines to be implemented and only 14% of interventions are impacting the intended patient population, physical therapist Lena Volland said at a recent NBDF webinar. She has hands-on experience providing PT at hemophilia treatment centers and she’s also NBDF’s Director of Education.
MASAC's strategies have their roots in research and expertise, but putting these guidelines into action is not always a straightforward task.
"There are many compounding factors that will prevent something from being implemented in the clinical practice," said Volland. For MASAC's recommendations to be fully effective, a well-planned and executed strategy for implementation is necessary.
Barriers to Implementation
NBDF surveyed physical therapists at HTCs about barriers that prevent the application of best practices recommended in the MASC guidelines. The survey found a high percentage of alignment with MASC guidelines – 82%. But an analysis of survey results also identified reasons why the treatment guidelines aren’t always followed. They included patient preference, limitations of the physical space in therapy areas, a lack of funding and problems with health insurance coverage.
Continuing education programs are necessary to spread specialized information, according to Volland. Experienced professionals can share their skills through mentorship programs, she said. Volland also noted that providing financial support for full-time physical therapist positions helps address staff limitations in hemophilia treatment centers.
Watch the webinar: Recommendations vs. Practice: Physical Therapy at HTCs